FAQ's - Neuromodulation Frequently Asked Questions
We have separated FAQ’s into four sections. Please click on the section that represents your needs: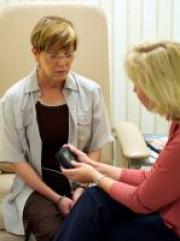
Patients
Q1 What conditions are neuromodulation techniques used to treat?
Neuromodulation is used to treat and enhance quality of life in individuals who suffer severe chronic illness due to persistent pain, spasticity, movement disorders, epilepsy, ischaemia, cardiac, bowel and bladder dysfunction, spinal injury, visual, auditory and specific psychiatric disorders.
The most common treatment is spinal cord stimulation and the most common indication is the persistent severe neuropathic pain found in those who have had technically successful spinal decompression surgery, but who have had recurrence or persistence of symptoms.
Q2 What is the procedure for patient assessment prior to implant?
The decision to provide a neuromodulation therapy is taken after careful consideration with you, your implanting doctor and the neuromodulation team. It is neither a treatment of first nor last resort. If symptoms can be managed effectively and simply using other methods then these are considered first.
Often your doctor will recommend that you see several other professionals in the multidisciplinary team before agreeing to do a neuromodulation treatment, in order to be really sure that this is the best treatment at the best time for you, and to decide if any additional therapy is required.
Q3 What is involved in the neuromodulation implant procedure?
Clearly the implant procedure is different depending upon the actual procedure done and by whom. Quite often the electrodes or catheters are placed under local anaesthetic.
Q4 What questions does the INS suggest I ask my implanting doctor?
You should ask your doctor about the neuromodulation treatment selected and whether there are any simpler alternatives or solutions to your problem. There will be advantages and disadvantages to any treatment, but it is important you should know as much as possible. You should ask about their track record with the treatment and what their rate of common complications is. You should ask who will be your long term contact in the neuromodulation team.
Q5 What are the side effects of these treatments?
There are complications that are general to any implant into the body and complications that are specific to the technique, therapy and disease. You should ask your doctor and the implanting team all about any common or dangerous possible side effects before embarking on this or any treatment. Further information on complications specific to the device, technique and therapy can be found from the manufacturers’ own websites.
Q6 If I undergo treatment, how long will it take me to recover and how long will I be off work?
The amount of time required off work following these treatments will depend upon several factors, and it would be best to check with the neuromodulation team.
Q7 Will my body reject the device after it is implanted?
The devices are made of materials that are usually well tolerated by the body. True rejection is extremely rare.
Q8 How long will the device need to be in me?
Due to the nature of your symptoms it is more than likely that you have a permanent condition. Thus, neuromodulation is usually embarked upon with the expectation that the system will be required long term. The simplest answer is to say for as long as you need it. However, the device can be removed.
Q9 What happens if the device breaks down?
Your implant team would need to be contacted. The problem can usually be diagnosed after asking you some questions and by interrogating the device with the master computer. Further action can then be advised.
Q10 How often will the device need to be replaced?
There are several components to the neuromodulation device. For advice on battery life please see question 12. Owing to the fact that these are mechanical devices there is a requirement for maintenance, as one might expect.
Q11 How is the device regulated once it has been implanted?
The fully implanted stimulator systems can be programmed using telemetry by your doctor’s programmer. Most of the newer devices will be issued with a patient programmer so that you will be able to not only turn it on and off but also make your own adjustments to the stimulation. The drug delivery systems will be adjusted if required by your doctor.
Q12 How long does the battery last?
Please also refer to the individual manufacturers’ websites.
There are now three ways that the stimulating devices are powered.
The newest devices are rechargeable systems. Longevity varies from nine years to more depending upon manufacturer and usage.
A commonly used system has an internal non-rechargeable battery which comes in various sizes.
Once this is exhausted the whole implantable pulse generator which includes the battery (IPG) is replaced. The longevity is variable. Typically we would expect an IPG to last between two and seven years depending upon size, manufacturer and usage.
The original systems, which may sometimes still be used in certain instances, are those powered by radiofrequency coupling, whereby power is transmitted continuously through the skin to the device from an external transmitter stuck to the surface of the skin. Typically these devices might last 7 years or more.
Some drug delivery pumps are powered electrically with an internal battery and may last seven to 10 years depending on manufacturer. Other pumps are constant flow rate and gas driven. The hydraulic pressure in the gas when compressed at refill powers the constant flow rate. These pumps may last longer than 10 years.
Please note: This information should not be used as a substitute for medical treatment and advice. Always consult a medical professional about any health-related questions or concerns.
Prospective Members
Q1 What are the benefits of INS membership?
The INS is the fastest growing, multidisciplinary and representative worldwide body dedicated to the scientific development and knowledge dissemination of neuromodulation. The INS provides leadership and a forum for clinical and scientific endeavour into this exciting and sometimes novel medical discipline. Full membership benefits are detailed in the membership section.
Q2 How do I join the INS?
Visit the membership page. Look to see if your country is represented by a chapter society, select the chapter in your region, and complete the online application form and payment information. If your country is not represented by a national chapter society, then simply select INS - Global and complete the online application form with payment information.
Q3 How much does membership cost and how does my membership fee get used?
Membership in the INS is $150 per annum, which covers the INS's operational expenses to offer its live and web-based educational programs, as well as the cost of its journal, Neuromodulation: Technology at the Neural Interface. There are discounted rates for student, nurse and allied healthcare professionals.
If you also join the chapter society there will be further benefits and costs which are detailed in the membership section.
Q4 There isn’t an INS Chapter in my region. What are my options?
You may note that in some parts of the world there are regional chapter societies in development; so after joining the INS please make contact with the lead person to see if criteria for national chapter society formation are met. You may also contact INS Executive Office.
Q5 Who is entitled to join the INS?
The INS is open to membership from all disciplines providing that the applicant has a substantial professional interest in neuromodulation.
Q6 How can I communicate with other INS members?
This website has secure areas for members. These areas can be accessed either via the INS website or your national chapter society website. This will provide discussion forums as well as email addresses for contact of individual members.
Q7 What events are organised and supported by the INS?
The INS holds a world congress every two years. Each national chapter society holds a scientific meeting annually. See INS Events Calendar for further details.
Q8 What sort of relationship does the INS have with the medical device and pharmaceutical industries?
The INS is a non profit organisation. The society is funded through a combination of membership dues, profits from journal and world congresses, and some unrestricted sponsorship grants from a broad portfolio of the medical device and pharmaceutical industries. The INS maintains commercial independence and its Conflict of Interest Policy is available here. The INS annual accounts are published and presented to the general meeting during the world congresses. They are available for public viewing via the Executive Office.
Q9 Are members of industry allowed to join the INS?
Individual members of industry who have a substantial interest in neuromodulation are entitled to join the INS.
Medical Professionals
Q1 What conditions are neuromodulation techniques used to treat?
Neuromodulation is used to treat and enhance quality of life in individuals who suffer severe chronic illness due to persistent pain, spasticity, movement disorders, epilepsy, ischaemia, cardiac, bowel and bladder dysfunction, spinal injury, visual, auditory and specific psychiatric disorders.
The most common treatment is spinal cord stimulation; and the most common indication is the persistent severe neuropathic pain found in those who have had technically successful spinal decompression surgery, but who have had recurrence or persistence of symptoms.
Q2 Where is the evidence base to support neuromodulation?
The scientific community members who are involved with neuromodulation have recognised the need to produce high quality evidence of clinical efficacy. Considering the difficulties in performing randomised controlled trials with surgical techniques much has been achieved, such as SCS for angina pectoris, critical limb ischaemia, complex regional pain syndrome and neuropathic failed back surgery syndrome. Similar quality has been achieved with sacral nerve stimulation for faecal and urinary incontinence, intrathecal baclofen in spasticity, intrathecal opioids in cancer pain and vagal nerve stimulation in epilepsy, and cochlear implantations.
Q3 What is the procedure for patient assessment prior to implant?
The decision to provide a neuromodulation therapy is taken after careful consideration with the patient, the implanting doctor and the neuromodulation team. It is neither a treatment of first nor last resort. If symptoms can be managed effectively and simply using other methods then these are considered first.
Q4 What is involved in the neuromodulation implant procedure?
Clearly the implant procedure is different depending upon the actual procedure done and by whom. Quite often the electrodes or catheters are placed under local anaesthetic. Other parts of the procedures can be more satisfactorily done under general anaesthesia.
Q5 How do I decide if neuromodulation is the best treatment for my patient?
There are many different indications for neuromodulation. All are agreed that these therapies fulfil the needs of patients at the niche end of a spectrum of disease severity and impact. However as good quality research trials accrue it becomes more likely that these therapies will be introduced earlier in traditional chronic disease management. Neuromodulation should be considered as part of a portfolio of management strategies and selected after multidisciplinary consideration and expert application and support.
Q6 What complications are associated with neuromodulation techniques?
There are complications that are general to any implant into the body and complications that are specific to the technique, therapy and disease. Each implanting centre will be monitoring these and should be able to quote their current rates of complication.
The weaker parts of the systems used tend to be the electrodes, catheters and connections. INS members are working hard with industry to improve design, and system durability.
Complications specific to the devices, technique and therapy can be found from the manufacturers’ own websites.
Q7 What are the costs and cost-effectiveness of neuromodulation?
There are several costs of the procedures to be considered. These are implant components, professional fees, operating room and hospitalisation costs. Cost effectiveness of the procedure is a method by which the total costs of the procedure as well as the change in healthcare costs following the procedure are compared with the costs of not providing the treatment. Various cost analyses have been done for some of the neuromodulation procedures for some of the indications. For example, SCS appears to become cost effective between 2 and 2.5 years after treatment in patients with angina pectoris, failed back surgery syndrome and complex regional pain syndrome.
Q8 Where is my nearest INS member’s clinic?
Those members that have indicated that they wish their clinic contact details to be made available can be contacted via the INS website or national chapter website.
Q9 I need to do further research in this area before I recommend a patient for neuromodulation. Where do you suggest I look?
There is a useful bibliography in this website which although not exhaustive, is a list of some of the more influential and well-received publications. Explanatory content on our therapies page often includes specific citations and references; as does material gathered on our overview page for medical providers. Also, texts and additional resources are listed on our links page. Finally, the end of the therapies page also lists evidence tables about investigational deep brain stimulation studies in certain behavioral or psychiatric conditions.
Commercial Interest
Q1 How do I present my company's products and services to INS members?
There are several ways of communicating to INS members. Advertising space can be purchased in the journal, Neuromodulation: Technology at the Neural Interface. For more information, please contact the executive office of the INS via contact us.
Q2 Is the list of INS members available to purchase?
No, the INS does not sell its members' data.
Q3 Are there opportunities to present my company’s products and services at INS events?
The INS holds a world congress every other year. Industry partners are invited to exhibit their products at these congresses. Satellite symposia can also be funded, providing they fit with the organising committee’s plans. Each national chapter society holds an annual scientific meeting to which industry partners are invited to exhibit and support.
Q4 I have a new product for clinical trial. How do I identify centres for clinical trials?
If you send your request to the executive office via contact us it will be cascaded to all national chapter administrators who will ensure that all sites interested in clinical trials are informed.
Q5 Can the INS suggest or arrange a speaker for our event?
If you send your request to the executive office of the INS via contact us it will be cascaded to the Full Board of the INS for consideration.
Q6 Can the INS help with suggestions of members for an advisory board?
If a global advisory board is required then please contact executive office of the INS via contact us who will cascade request to the Full Board of the INS for consideration. If it is for a national advisory board then please contact the relevant national chapter.
Q7 What is the Advanced Medical Technology Association (AdvaMed) Code of Ethics, and where can I find it?
To help to continue to assure a high standard of ethical conduct by the medical technology industry, AdvaMed offers its own ethical guidelines for the medical technology industry, which underwent an update to take effect in 2020.
"The Code of Ethics for Interactions with Health Care Professionals" was approved by the Board of Directors in September 2003 and became effective January 1, 2004. (Download PDF)
Executives, sales, marketing, finance, medical affairs and legal staff from medical technology firms, as well as physicians, hospital administrators, group purchasing organizations, dealers and distributors should all thoroughly understand the impetus for changes in these ethical guidelines and how organizations and individuals alike are expected to conform.
|

